Ballarat Orthopaedics & Sports Medicine - Joint Replacements
At Ballarat Orthopaedics & Sports Medicine, we have experience in a breadth of joint replacement.
USEFUL INFORMATION
Joint Replacement Options & Information
Non operative treatments of hip arthritis
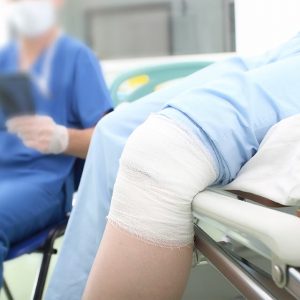
Not every arthritic joint needs a joint replacement, or at least might not need it yet. Non-operative treatments such as medications (analgesics and anti-inflammatories) or an injection into the joint have a useful role for some patients. Especially where the patient is relatively young, or the joint not grossly arthritic, it may be possible to resume almost full activity with these treatments.
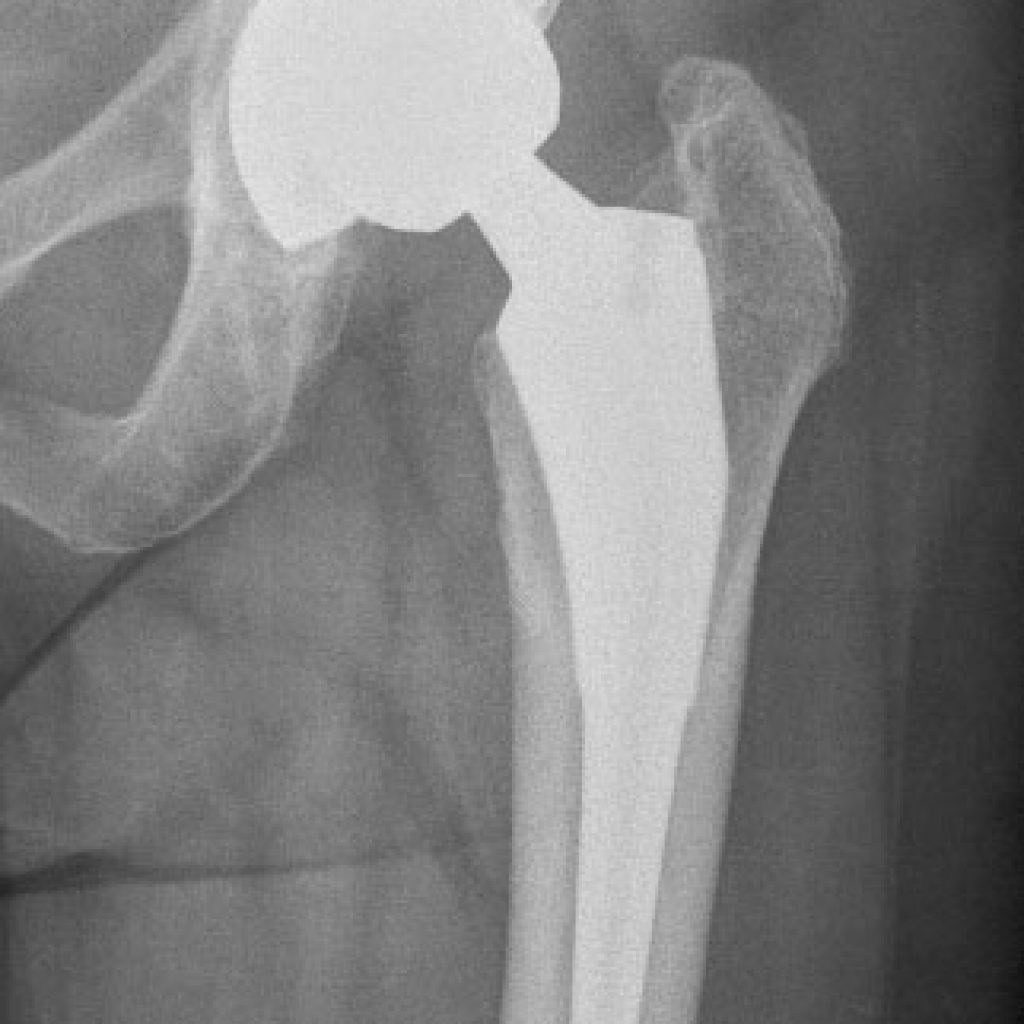
Conventional Hip Replacement
The hip is a ball and socket joint. Since Sir John Charnley came up with a reliable method of fixing a new ball and socket in 1958, and then from 1962 using polyethylene, hip replacement has progressively become mainstream surgery. The current techniques allow rapid recovery – the majority of patients will walk on the day of surgery and be ready to go home the day after. Some elderly frail patients may need to spend some time in rehabilitation, but this group is only 2% or so of our patients, and we will identify those patients at a preadmission appointment.
Patients usually go home using a single elbow crutch, and are advised to walk every 1-2 hours during daylight hours. There is no reason to be “housebound” assuming the ground outside is relatively safe. It is better if there is someone at home – not to nurse you – but provide company.
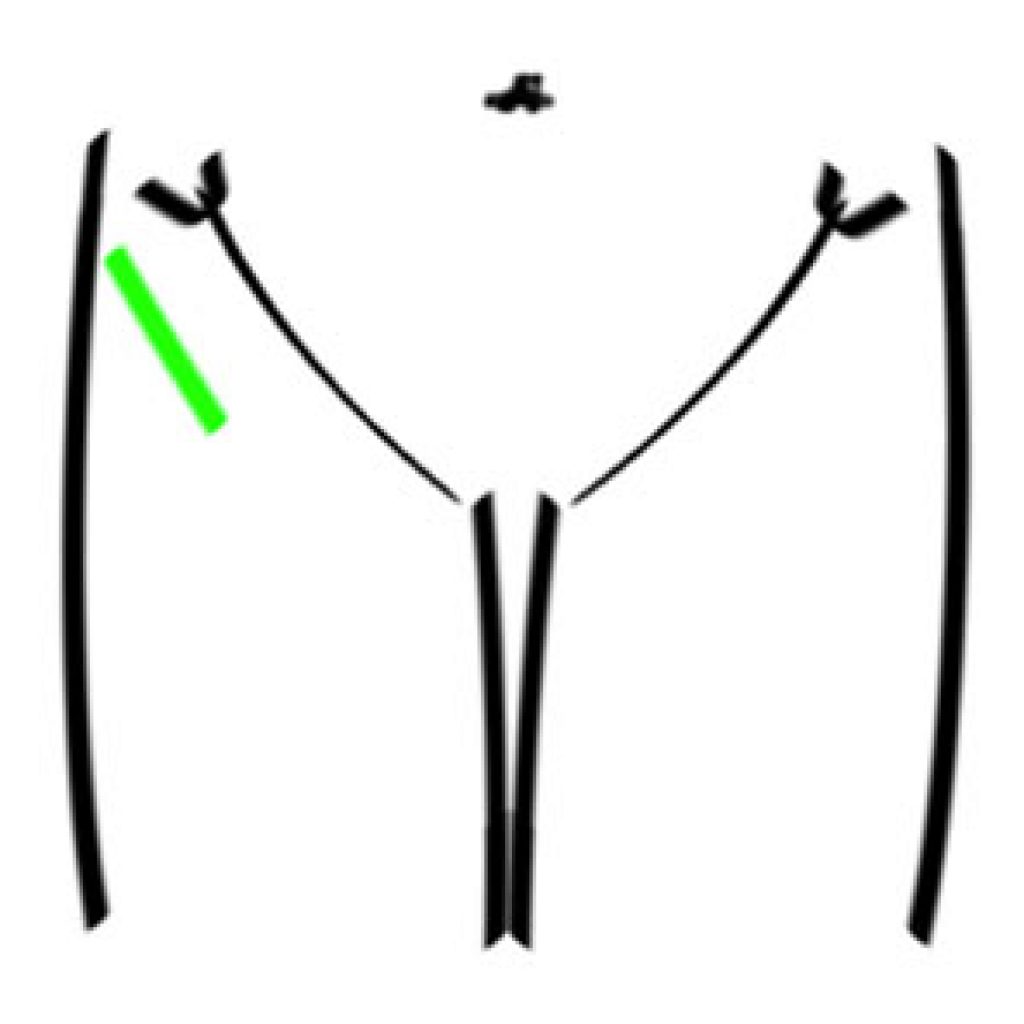
Anterior approach hip replacement
The most common approach in Australia – the “posterior approach” – is being challenged with a new approach – the “anterior approach”. The Australian Arthroplasty Society has a statement that surgical approach does not influence results. The risk – benefit equation is critical.
Anterior approach theoretically may reduce the dislocation rate, and may speed up recovery. The question is whether it increases the risk of what were rare complications – fracture, or possibly infection. A thin, ligamentously lax patient has the most to benefit from an anterior approach. Different incisions can be used, this “Bikini” incision heals beautifully in thin people as it is parallel to “Langers lines” and avoids getting to close to the boney prominence. A similar scar starting at the same site but angling towards the outer kneecap can be used in heavier patients.
Our surgeons can talk to you about both approaches.
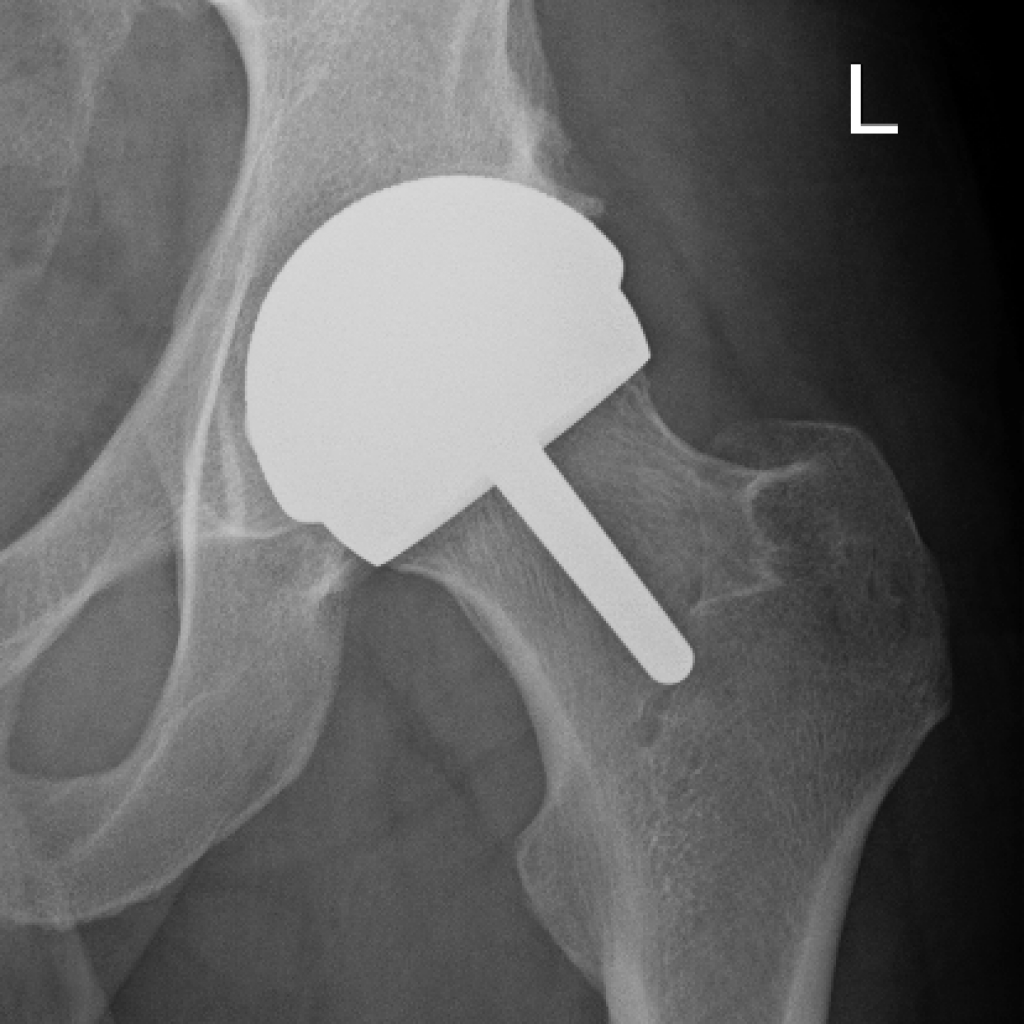
Hip Resurfacing
Birmingham, although the ceramic-ceramic resurfacings are showing promise, and are now available in Australia. The preferred patients have good bone quality, are of normal weight and height typically over 170cm in order to fit the sizes that are proven.
The surgery is more complex that hip replacement, the surgeon needs above average results to justify resurfacing.
Advantages of Hip Resurfacing
- Industrial strength operation
- exceeding low incidence of dislocation
- More accurate leg length
- Lowers risk of blood clot complications
- Lower risk of thigh pain
Non operative treatment of arthritis
Knee Replacement
The knee is a complex hinge joint. Since Insall & Bernstein introduced their total condylar knee replacement in 1974, knee replacement has progressively become mainstream surgery. The current techniques allow rapid recovery – the majority of patients will walk on the day of surgery and be ready to go home the day after. Some elderly frail patients may need to spend some time in rehabilitation, but this group is only 2% or so of our patients, and we will identify those patients at a preadmission appointment.
Patients usually go home using a single elbow crutch, and are advised to walk every 1-2 hours during daylight hours. There is no reason to be “housebound” assuming the ground outside is relatively safe. It is better if there is someone at home – not to nurse you – but provide company.
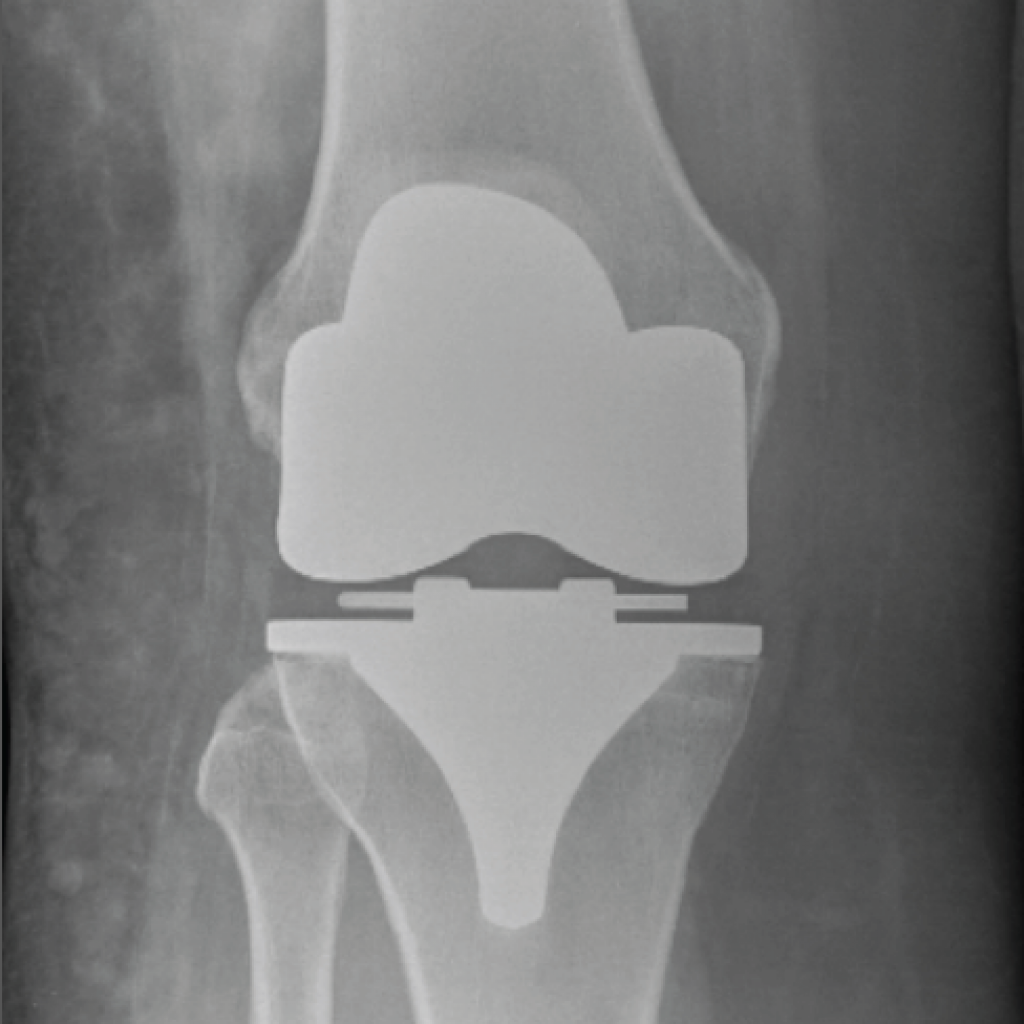
Partial Knee Replacement
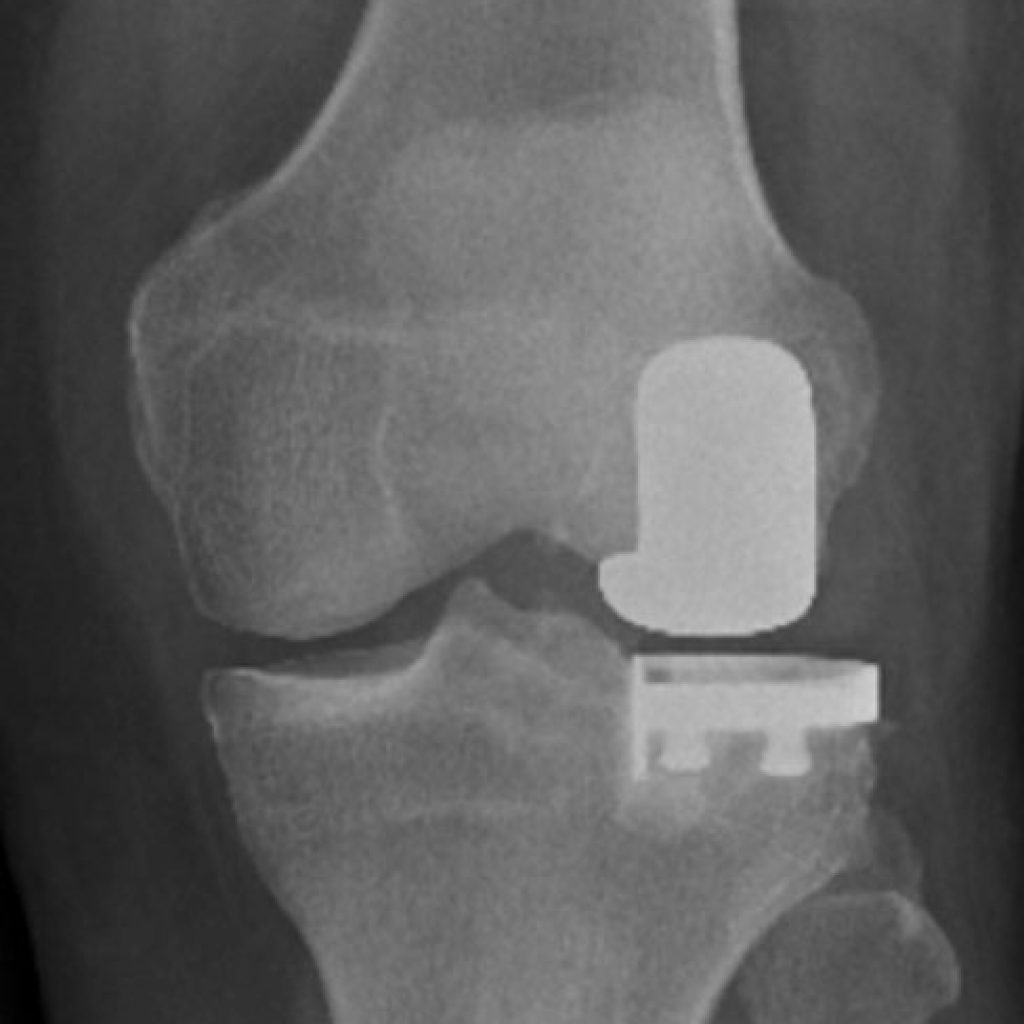
Shoulder – Non Operative Treatment
Non-operative treatments can include paracetamol, anti-inflammatory medications and activity modification. Modifications include moving objects from overhead cupboards into easily accessible ones, and the use of clothes dryer & clotheshorse.
Before seriously considering shoulder replacement, it is important that these simple non operative treatments have been undertaken which clearly have less risk than surgery.
Shoulder Replacement
Shoulder arthritis alone is less common surgery than hip or knee replacement. None the less, good designs are available, and the success of them in the Australian Joint Replacement Registry seems to be reasonably good, 93.6% continuing to function well at 7 years from surgery.
Shoulder replacement replaces the surface of the shoulder blade (glenoid) with a curved polyethylene surface, and a new ball replacing the surface of the upper arm (humerus). A titanium or metal stem within the upper humerus secures it to bone. Shoulder replacement relies on the surrounding tendons to balance the “ball and socket”.
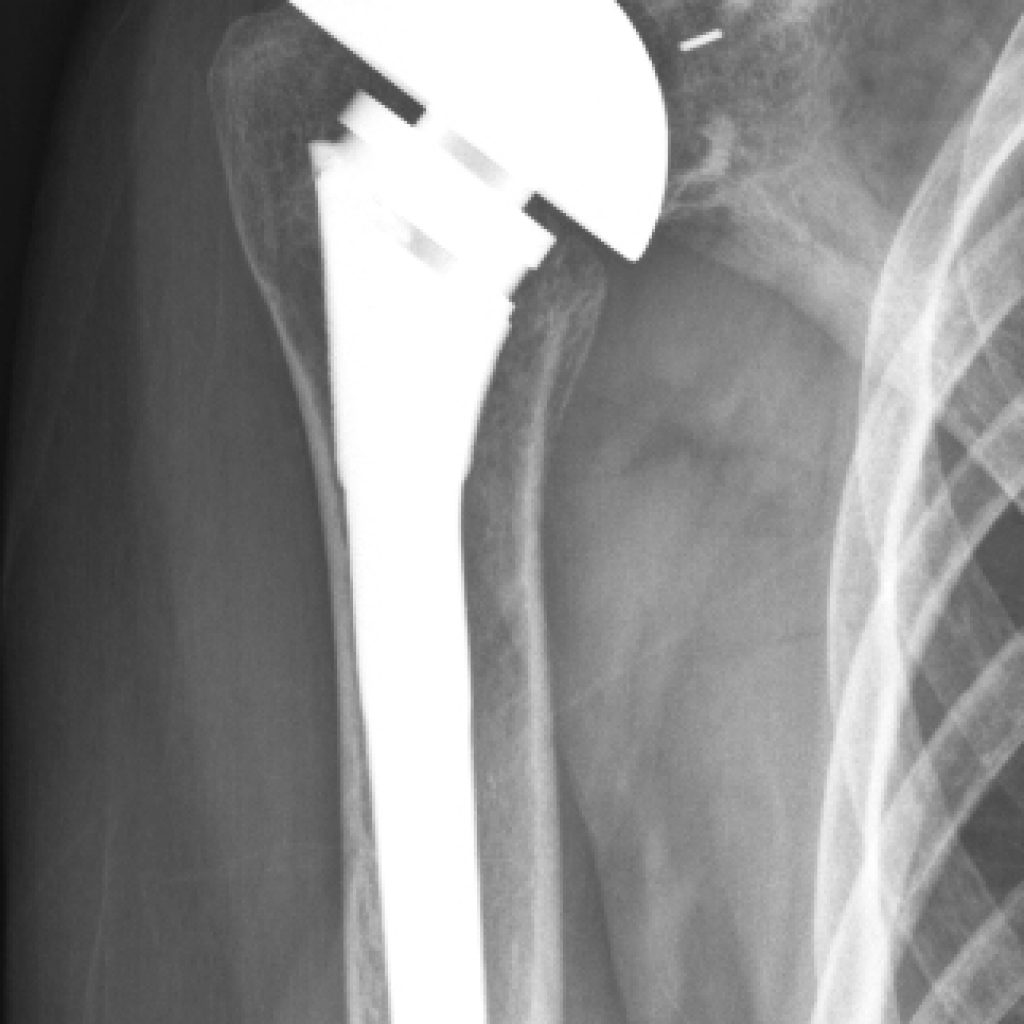
Reverse Shoulder Replacement
With an ageing population, it is apparent that long standing torn tendons in the shoulder can lead to arthritis. Pain and weakness are the most common reasons for a referral to an orthopaedic surgeon for treatment. The inability to usefully move the arm is called “pseudo paralysis”.
A reverse shoulder replacement is an interesting engineering feat. By swapping the ball to the glenoid side of the shoulder joint, the deltoid muscle is able to function without the underlying rotator cuff tendons. The deltoid muscle is the main muscle required to lift one’s arm overhead – so the pseudo paralysis is treated.
Reverse shoulder replacements are doing well in the Australian Joint Replacement Registry, which in 2016 was tracking the progress of 12362 patients across the country. At 7 years from surgery, only 4.7% have come to further surgery. One of the factors in this is probably that reverse shoulder replacements are often done in older patients, more than 50% of the operations are done in patients over 50 years of age.
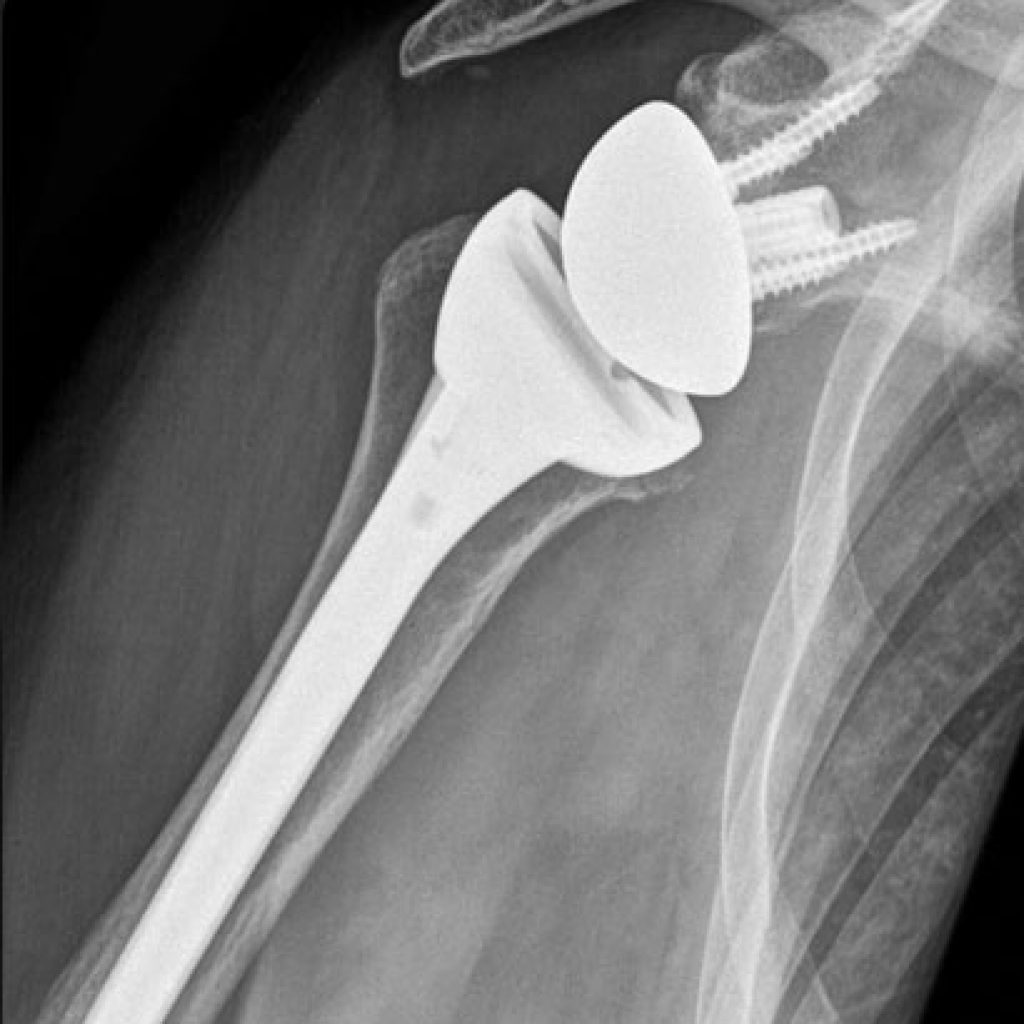
Ankle – Non Operative Treatment
Non-operative treatments can include paracetamol, anti-inflammatory medications and activity modification. An ankle brace to support it during activity, or lace up boots may diminish the pain.
Weight reduction may be necessary for some patients. Before seriously considering any of the reconstruction operations, it is important that these simple non operative treatments have been undertaken which clearly have less risk than surgery.
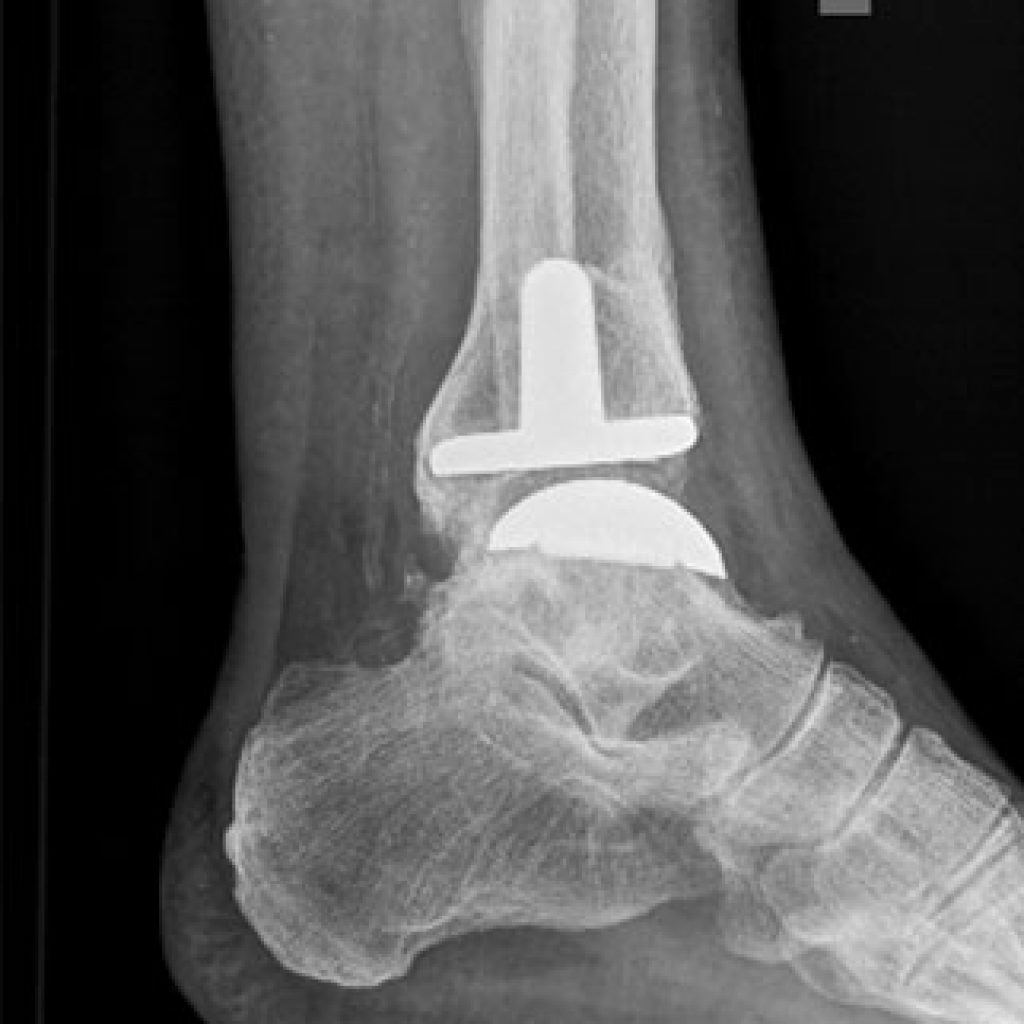
Ankle replacement
Ankle replacement is a rarely performed operation, the results are not as good as hip or knee replacement, and the solutions for failed ankle replacement are all drastic. For this reason, most patients are better to have ankle ankle fusion.
Ankle replacement might be considered in an elderly patient with good bone quality, and a reason that ankle replacement may not be so good such as arthritis of the joint below the ankle as well.
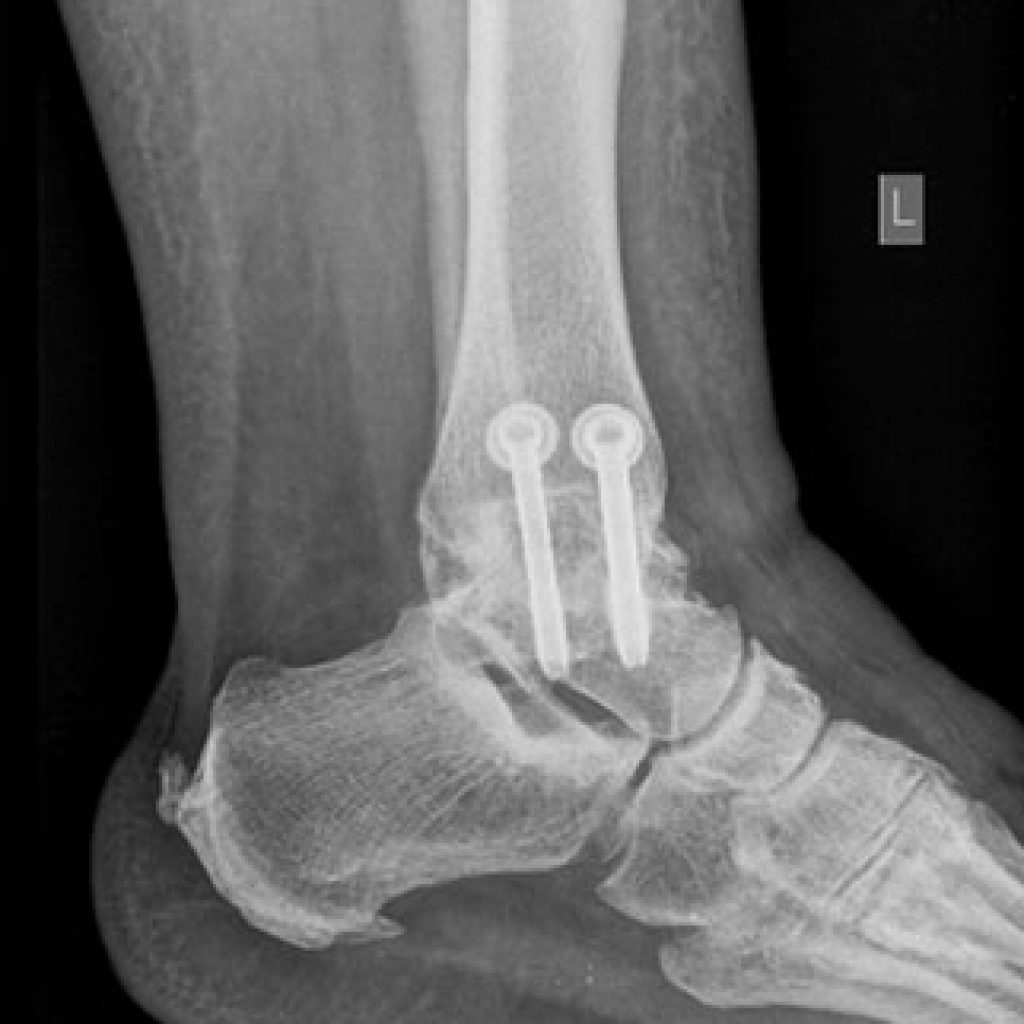
Ankle Fusion
A more robust operation with a higher success rate for ankle arthritis is ankle fusion. A fusion operation is where the arthritic joint surfaces are removed, and the underlying “cancellous” bone surfaces compressed together with screws.
The operation is usually done arthroscopically, with a single night in hospital. A plaster cast is required to protect the fusion, and then a cam boot or “moon boot” until the fusion is solid at three months. Some “up-down” movement of the foot is still possible after the surgery as the next series of joint contribute some movement in that direction.
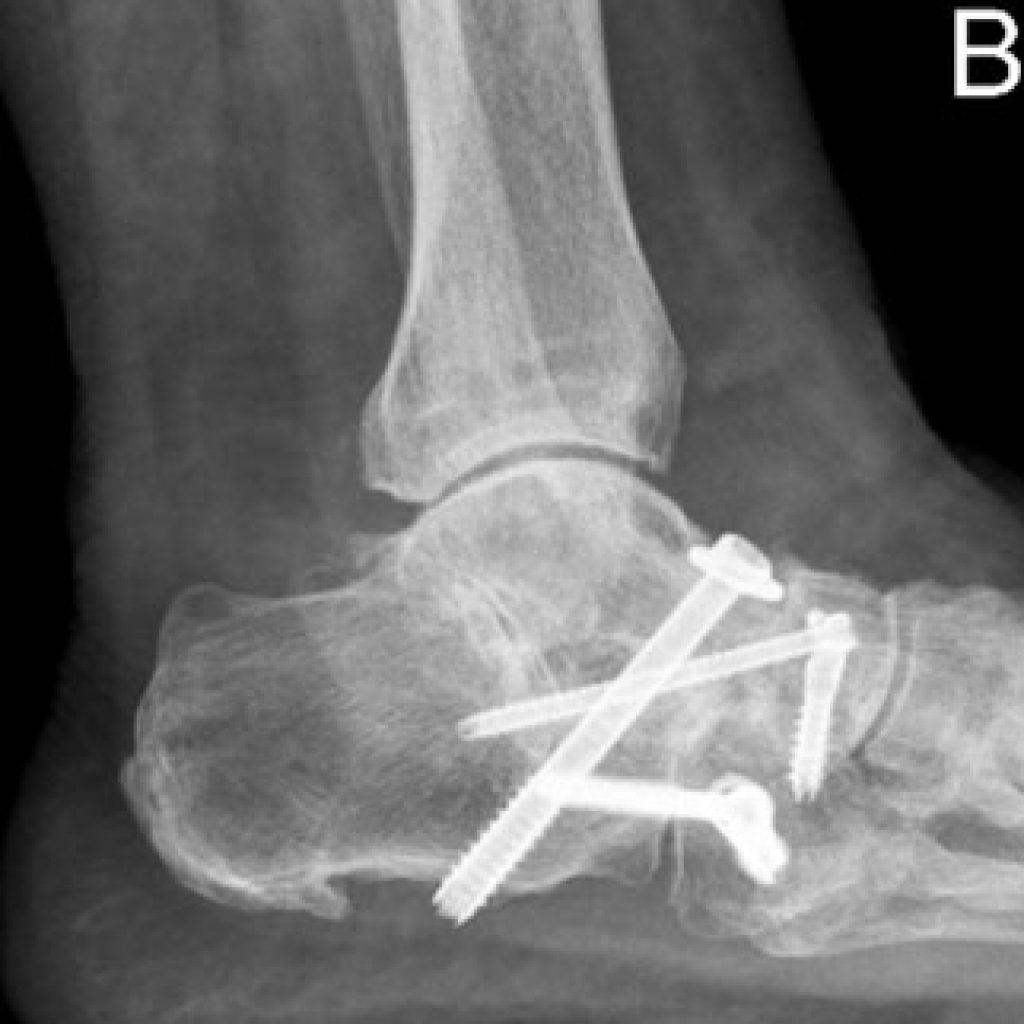
Triple arthrodesis
Almost as common as ankle arthritis is arthritis of the next series of joints below the ankle the do the “in-out” movement that allows one to walk across a slope. The three joints move together, so when arthritic, often all three are involved.
Like other fusion operations, the joint surfaces are removed, and the cancellous bone surfaces are compressed together. Bone graft may be required especially if there is a significant deformity. Like ankle fusion, a plaster cast is used initially, then a cam boot until about three months from surgery.
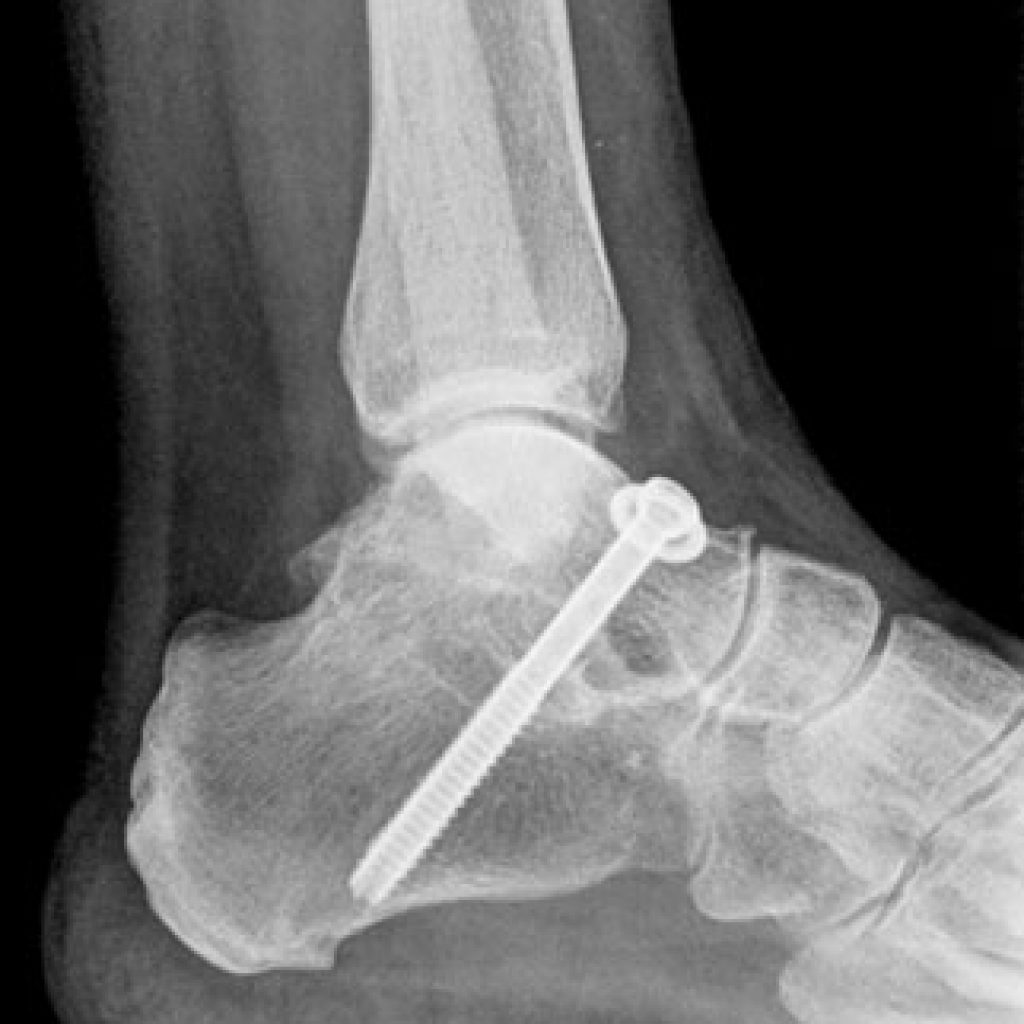
Subtalar arthrodesis
Elbow Replacements
Leading Treatments & Surgeries in Ballarat
- All
- Sports Medicine
- Orthopaedics
- Novar Specialists