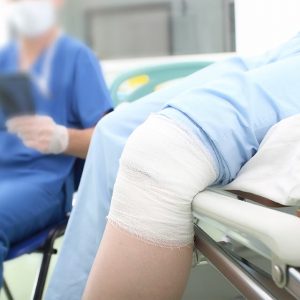
Ballarat Orthopaedics & Sports Medicine - Knee Surgery
Ballarat Orthopaedics & Sports Medicine are knee specialist in Ballarat with experienced and fellowship trained surgeons for your procedure.
The knee is the largest joint of the body and is also the most complex. It connects the thigh with the rest of the leg and supports all of our weight through a huge range of movement. The ligaments hold it steady during twisting and pivoting movement.
The complexity of the knee surgery depends on what portion of the knee needs to be treated and what type of repair needs to be performed. Operating can be done to repair damage, or prevent further injury.
Useful Information
-
Novar Specialist Healthcare
109 Webster Street
Lake Wendouree VIC 3350 - T | 03 5332 2969
- F | 03 5332 2003
- admin@ballaratosm.com.au
Knee Surgery Options & Information
Knee Arthroscopy
Arthroscopy is a minimally invasive surgical procedure that involves using small portals into a joint.
These small incisions allow the surgeon to fix a variety of problems. They allow the surgeon to insert a fibre optic camera and specialty instruments to examine the joint, and carry out a range of treatments. It is typically done for symptoms such as pain, swelling, locking, catching, and sometimes “giving way”. Most arthroscopic procedures are performed as day cases.
Problems rectified with arthroscopy include:
- Meniscal (commonly known as cartilage) tears
- Meniscal repairs in certain cases
- Removal of loose bodies
- Haemarthrosis after patella dislocation
- Osteochondritis dessicans
- Patella problems
Arthroscopy is used as part of more complex procedures such as:
- ACL reconstruction
- Realignment osteotomy
- Patellofemoral realignment
- Meniscal transplant
Knee Arthroscopic Meniscectomy
Knee arthroscopy is a camera controlled operation. Meniscectomy refers to removing part of a torn cartilage.
The cartilages function as shock absorbers between the thigh bone (femur) and the shin bone (tibia). They can be damaged through unusual forces (eg sporting injuries) in young people, and minor forces (eg squatting) in older people.
There are many instances that cartilage repair is the best operation, but probably in 90% of cases, the cartilage can’t be repaired. If it is a small tear causing minimal symptoms, the decision could be to leave it. If it causes severe night time pain, causing the knee to swell, or making the knee unreliable, then surgery to remove the torn fragment may be the best plan.
Most cases are typically done as day surgery, typically under general anaesthesia. Most patients do not require crutches afterwards, and are reasonable functional the day after surgery.
Removing even a small amount of he cartilage changes the forces in the knee, but in truth, the torn cartilage wasn’t preventing arthritis from occurring anyway. However, further injuries to the knee in the future might not be so easily treated.
Repeated “arthroscopic clean ups” should be unusual. Depending on patient needs, sometimes meniscal transplant, realignment surgery or even partial or total joint replacement should be considered instead.
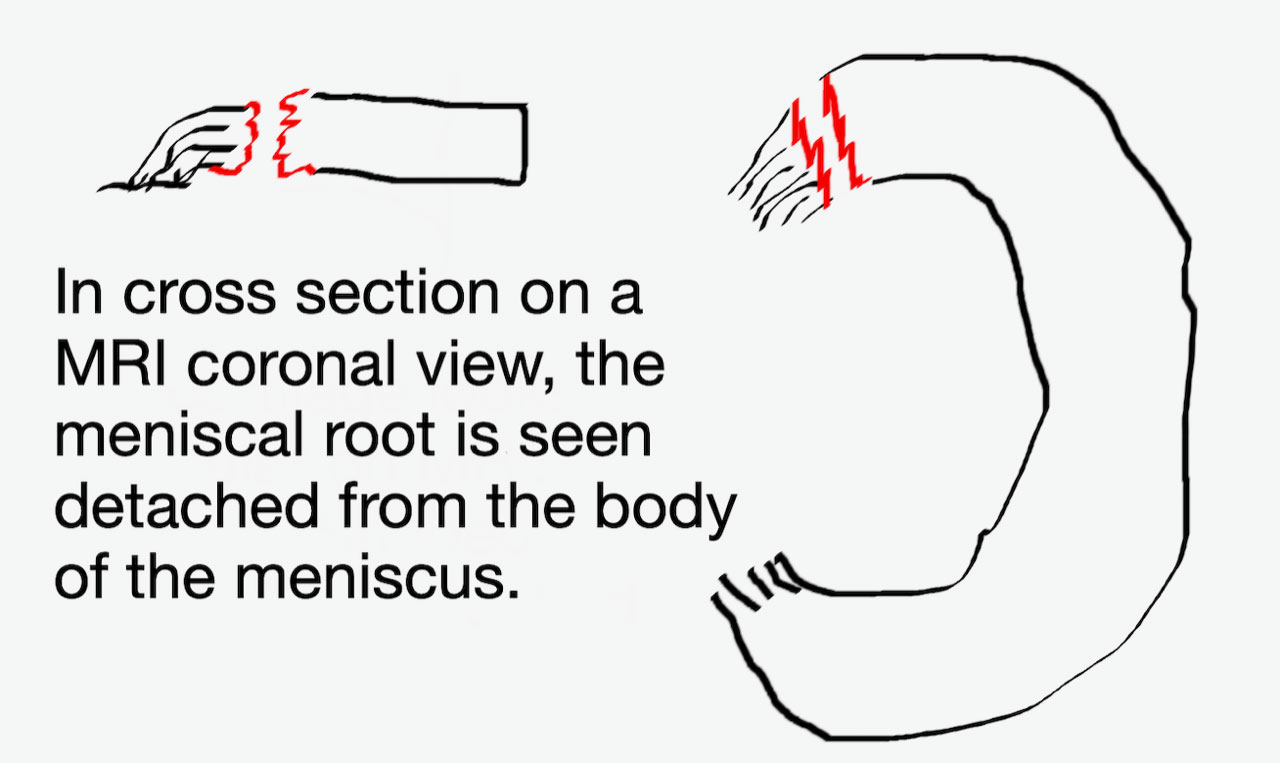
Knee Arthroscopic Meniscal Repair
Meniscal repairs have come along in leaps and bounds with better understanding of the pathology and which tears have best potential to heal.
New tools have come available to repair lesions previously felt irreparable, and concomitant surgery (eg cruciate reconstruction, MCL pie crusting) is often necessary.
Certainly there is a more difficult recovery after the surgery than simple meniscectomy, but for the right cases, the success rate is high, and final result better.
Successful meniscal repair protects the knee in the long term.
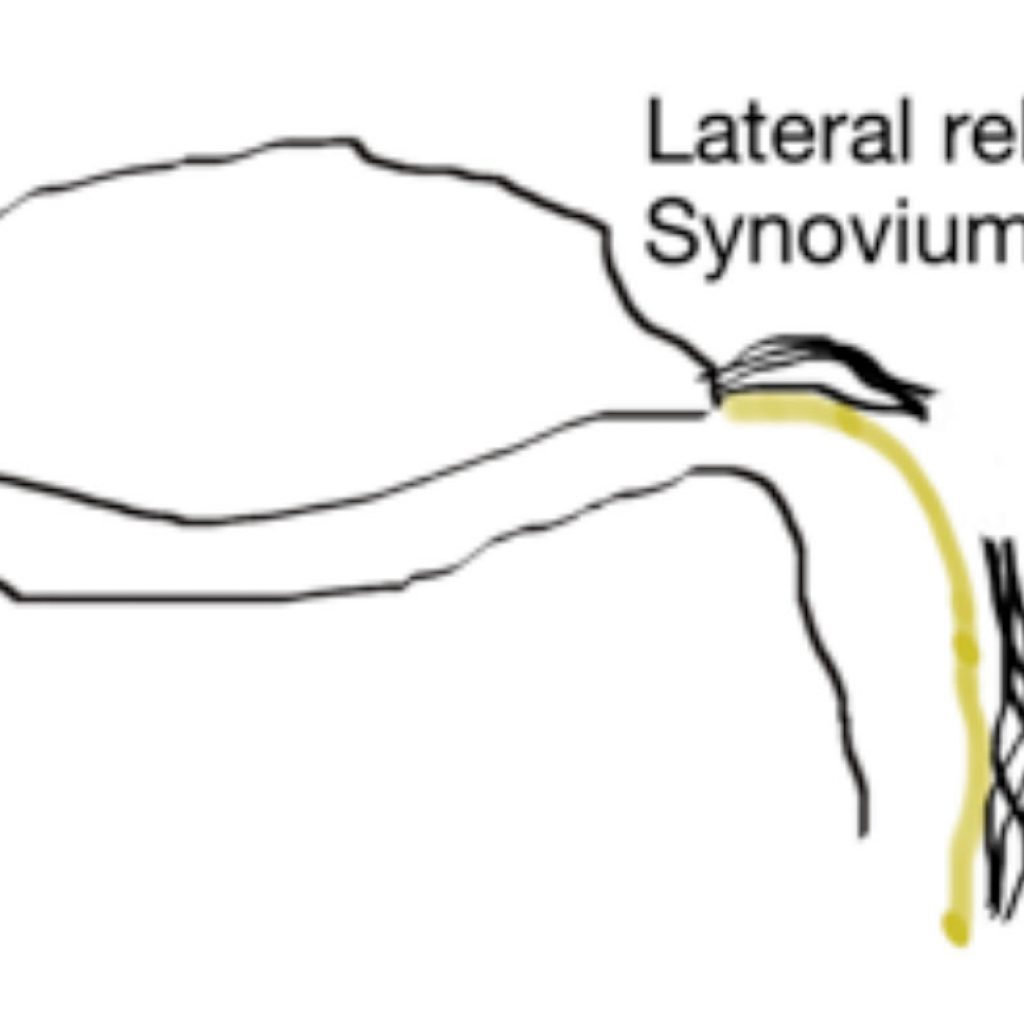
Arthroscopy & Lateral Release
In a normally functioning knee, the kneecap (patella) is exposed to forces some 9 times the body weight with normal activities – eg climbing stairs and getting out of a chair.
These forces are higher again with sporting activities. The lateral retinaculum provides a “check reign” to avoid the kneecap moving too far from its normal position.
If the kneecap isn’t “tracking normally” in the groove in the front of the femur (the trochlear) then the forces are higher again. Physiotherapy, ITB stretching, taping, and VMO strengthening carry a 90% cure rate – so most patients need physiotherapy, not surgery. The VMO is a muscle on the inner aspect of the knee that usually helps keep the kneecap in place. If it becomes weak, it needs to be strengthened.
The recalcitrant cases – where pain persists for months despite good physiotherapy – may be suitable for lateral release – lengthening the structure pulling the kneecap outwards, and thus spreading out the pressure on the kneecap. This is relatively minor day surgery requiring crutches only a few days, back to physio, then back to sport.
Knee Arthroscopy & Arthritis
Symptoms such as locking, catching, and sometimes giving way may be able to be improved by arthroscopic surgery even in the presence of arthritis. Osteoarthritic aching cannot be reliably rectified through arthroscopic surgery, but small areas of damaged joint surface can be improved.
Arthroscopy may be used as part of a more complex procedure such as:
- Realignment osteotomy
- Decision making on whether a knee is suitable for partial knee replacement
Procedures done in the presence of arthritis:
- Removal of loose bodies
- Chondroplasty
- Microfracturing
- Drilling
- Lateral release
Knee Replacement Surgery
Knee replacement is undertaken for end stage arthritis. The majority of people will have osteoarthritis caused by old injuries, bow- legs, knock-knees or being overweight. Rheumatoid and other forms of inflammatory arthritis can also damage the knee.
Symptoms of arthritis include pain, stiffness, swelling, catching or locking. Disabilities refer to the things you can’t do. For example – being unable walk a certain distance, difficulty getting out of a chair, or climbing stairs. From a personal level it might be that you can’t work, play bowls, or golf.
Before undergoing a knee replacement it’s important to have a severe enough problem that the benefit of surgery exceeds the risk involved. Non-operative treatments require patients to strive towards being strong, supply and slim. Exercise, tablets, braces, physiotherapy may be able to defer surgery to a later age, reducing the chance of reoperation in the future.
All members of our group use Local Infiltration Analgesia, reducing postoperative pain and allowing early mobilisation and its advantages. The proponents of this employ additional techniques to achieve Rapid Recovery Surgery where a single night in hospital is possible.
Knee replacement surgery can be
- Total knee replacement
- Mako Robotic knee replacement
- Partial knee replacement
Anterior Cruciate (ACL) Reconstruction
The anterior cruciate ligament is commonly injured in sporting accidents; the ligament is needed to keep the knee stable when twisting.
Depending on the degree of injury and level of sport, reconstructing the cruciate ligament might be advised.
The common reconstruction method in our practice is using your own hamstring tendons or quadriceps tendon. Particularly for revision cases and multilligament cases – , we also offer other techniques using allograft.
We adhere to the advice of the Australian Knee Society that in the majority of cases, a biological graft is available and preferable. It is exceedingly rare for us to recommend the artificial ligament called the LARS.
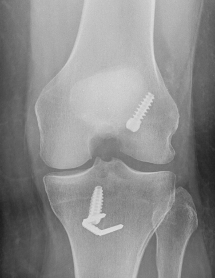
X-ray after a cruciate reconstruction
Multi-ligament knee injuries
The knee ligaments allow the smooth cartilage surfaces of the knee to remain stable during range of motion, impact, and pivoting/twisting activities. Ligaments are the tissues that join one bone to another.
High-energy knee injuries can lead to devastating consequences for stability, from injuries to more than one of the critical knee stabilisers. Multi-ligament knee injuries are very serious. With severe injury the entire knee can even dislocate and lead to tearing and damage to the nerves and even blood vessels. This can cause critical damage to the blood supply of the leg requiring vascular operations or potentially amputations.
Tendons join muscles to the bone. The knee has multiple ligaments and tendons. The major ones include the: anterior cruciate ligament (ACL), posterior cruciate ligament (PCL), medial collateral ligament (MCL), fibula collateral ligament (FCL), postero-lateral corner (PLC), anterolateral Ligament (ALL) and posterior oblique ligament (POL). The postero-lateral corner includes the FCL, Popliteo-fibular ligament and Popliteus tendon.
Knee Arthroscopic Meniscal Repair
The kneecap helps you to straighten your knee. It attached to your strong quadriceps muscle and to your leg bone (tibia).
It runs in a groove in your thigh-bone (femur), called the trochlea groove. Its bony shape, and the ligaments and muscles to which it is attached stabilise it.
The medial patello-femoral ligament (MPFL) can rupture after traumatic patella dislocation. This on its own can lead to ongoing feelings of kneecap instability.
Osteochondritis Dessicans (OCD) of the knee
During development, cartilage is slowly replaced by bone. This leaves a thin shell of smooth joint surface lining cartilage that covers the underlying bone.
In infants, what will become “bone” around joints starts off as cartilage. The cartilage is slowly replaced by bone through childhood except for a thin shell of smooth joint surface lining cartilage.
Occasionally, a piece of the underlying bone cracks with the overlying cartilage remaining intact in which case it may be a stable OCD lesion which will heal. However, when the overlying cartilage separate with the bone, joint fluid can wash under the bone and prevent bone healing (unstable OCD lesion).
In severe cases the bone and cartilage fragment can become loose within the joint. The most common joint involved is the knee, but also the ankle and elbow can be affected.
This process occurs during development, usually around the ages of 10 to 15. The younger the onset, the more likely the lesion will heal on its own, with restriction of activities and sports for a period of 6 months or more. A larger lesion presenting at a later age is less likely to heal on its own.
Knee Realignment Surgery
Knees that are “out of alignment” are more prone to arthritis. Depending on the severity of the situation, correcting the deformity can slow or stop the progression to arthritis.
The most common alignment problem in our society is bow legs, and this is most commonly corrected in the tibia with a “High Tibial Osteotomy”. The intention is to use rigid fixation and allow early weight bearing. In patients with early arthritis, they are commonly off crutches in two weeks. In more advance arthritis, it might take as long as six.
Knock-knee deformity is usually predominantly in the femur, the surgery corrected with a distal femoral osteotomy. In children, part of a grown plate can be slowed down using an “Eight Plate” achieving the same correction before arthritis has occurred. In young adults with pain, a realignment osteotomy can stop the progression of arthritis, and achieve return to sport.
Meniscal Transplants
Meniscal repairs have come along in leaps and bounds with better understanding of the pathology and which tears have best potential to heal.
It protects this cartilage by sharing the weight, acting as a cushion between the two sides of the joint and increasing the conformity of the joint.
Without a functioning meniscus there is an increase risk of developing wear and tear of that smooth joint surface cartilage. When this wear is significant it is called arthritis.
Cartilage (Chondral) Defects
The knee joint consists of your thighbone (femur) joining with the main leg bone (tibia). The kneecap (patella) also joins with the femur at the front. These bones are lined with a smooth joint cartilage (articular or hyaline cartilage) that allows pain free, and easy gliding, movements.
The shape of the joining bones does not completely match, as this allows some side-to-side and rotational motion. The spaces between the joint cartilage are filled with a cushioning cartilage (meniscus).
The meniscus is C shaped when viewed from above and triangular when viewed in cross section. The main function of the meniscus is to protect the important smooth joint lining cartilage.
There is a small amount of joint fluid that lubricates the joint and provides nutrition to the cartilage in the joint.
Other structures in the knee include the ligaments (that provide stability to the knee throughout its range of motion), and tendons (that connect the muscles to the bones to power the joint movement).
Patella Pain Surgery
In a normally functioning knee, the kneecap (patella) is exposed to forces some 9 time the body weight with normal activities – eg climbing stairs and getting out of a chair. These forces are higher again with sporting activities.Surgical options depend on how big an area of wear, how thick the wear is, the age and the needs of the patient. Options might be from simple day surgery lateral release, through to anteriorising Fulkerson osteotomy, even chondrocyte grafting. In older patients – partial or total knee replacement might be considered.
Leading Treatments & Surgeries in Ballarat
- All
- Sports Medicine
- Orthopaedics
- Novar Specialists